MIND BODY CONNECTION
The gut brain connection is actually fairly intuitive if you think about it-have you ever had “butterflies” in your stomach? Or even nausea after a very stressful experience? It’s evident even in the language we use- “I feel it in my gut” or “that scared me sh**less” (HA). This intimate relationship we’ve discovered between the gut and the brain embodies what we’ve always known as the “mind body connection”.
The gut actually has more neurons (nervous system cells) that the spinal cord itself (over 100 million!). Also in utero, the brain and the gut actually develop from the same tissue. Crazy right?! That is why your gut is considered your “second brain”, because not only is it a major part of your peripheral nervous system, but it can actually work autonomously from the brain.
A huge piece of the gut brain connection puzzle is the microbiome itself. The bacteria in your gut can produce and release neurotransmitters, just like our neurons do, and facilitate much of the function of the “GI or enteric nervous system”. The majority of many calming and happy neurotransmitters we rely on for good moods (GABA, serotonin, dopamine, etc.) are actually produced in the gut! Therefore seeking balance between the good and “bad” or opportunistic bacteria in the gut is essential for healthy neurotransmitter balance.
The brain and the gut are connected via a long nerve called the vagus and signals are sent in both directions along this “wire”. Interestingly though, about 80% of the communication via this nerve is from the gut to the brain. That means your gut is sending more messages to the brain than the brain is sending to the gut. You can imagine what implications that might have for mood and brain activity!
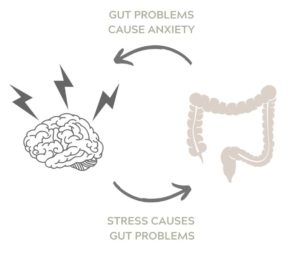
But, even though the gut is sending lots of messages to the brain, its still a two lane highway. It is very important in practice to address and balance both sides of the equation because-not only do brain troubles affect the gut (hello stress!), but gut troubles can also affect the brain. Therefore for example, a person’s GI issues or microbiome imbalance can be the cause or the product of anxiety, stress or depression, which can turn into a vicious cycle. Not only can the dysbiosis in the gut cause feelings of anxiety, depression and even addictiveness, it also can affect cognition, memory, and critical thinking skills (brain fog anyone?).
6 WAYS TO IMPROVE GUT HEALTH:
1– Reduce your stress. Chronically circulating stress hormones actually negatively alter the diversity and balance of your gut microbiome, which can give opportunity to pathogenic bacteria. Take the time you need to rest and recharge. Get some gut healthy self care on the calendar each week-like therapy, meditation, breathwork, smart & joyful exercise, and good sleep.
2-Eat a Diversity of Plants. Plant fibers in your diet selectively feed the good bacteria and help them thrive. They in turn decrease inflammation and keep the gut lining strong. Make sure you are eating a wide variety of foods that contain prebiotic fibers- This could include complex carbs like roots, tubers, seeds, garlic, onions, asparagus, leeks, bananas, legumes, etc. Aim to eat 40 different plant based foods a week an choose a variety of colors. If eating a diversity of plants causes gut issues, it’s time to get testing to figure out what’s going on and learn how to reintroduce.
3- Avoid exposure to pesticides, glycophosphate. This one may be controversial. However, scientists are making correlations between microbiome health and environmental toxin exposure. Avoiding pesticides like glycophosphate and antibiotics in meat and dairy products may be beneficial. However, I think eating a balanced diet rich in plants and whole foods will have great health benefits, even if those foods are conventionally grown or produced. I personally prioritize organic because it’s generally the eco friendly choice, but YOU have to choose whats right for you and your family.
4-Avoid unnecessary use of Antacids, PPI’s, Tums, NSAID’s, and antibiotics. According to the CDC at least 30% of antibiotics that are prescribed are not needed (And personally I think that is conservative). Antibiotics aren’t the only medications that kill or inhibit growth of good gut bacteria-PPI’s, Tums and other antacids also need to be considered. Lowering the stomach acid is like leaving the door open for opportunistic or pathogenic bacteria to get a foot hold in the lower GI. Not to mention these medications are often prescribed inappropriately as well. Last but not least the commonly used NSAIDs (like ibuprofen)- for even as little as five days in a row can lead to gastritis, ulcers, and leaky gut or altered gut permeability. Do you gut lining a favor and try to limit your use of these pain killers as much as you can.
5-Avoid sugar and artificial sugars in excess: Think of excessive sugar feeding the “bad bugs” in the gut, allowing them to proliferate and crowd out the good guys. Artificial sweeteners aren’t a great alternative unfortunately (I guess the fake, processed version never is), since they lead to leaky gut and dysbiosis as well. So I say, treat yourself with real sugar in moderation without guilt.
6-Start probiotics directed by your provider. Remember, not all probiotics products are created equal and include probiotic rich foods in your diet (ie: kimchi, kombucha, sauerkraut, miso, tempeh, etc.). Supplementing with probiotics is almost useless IMO if you don’t feed them with a diverse diet. So work on that first!